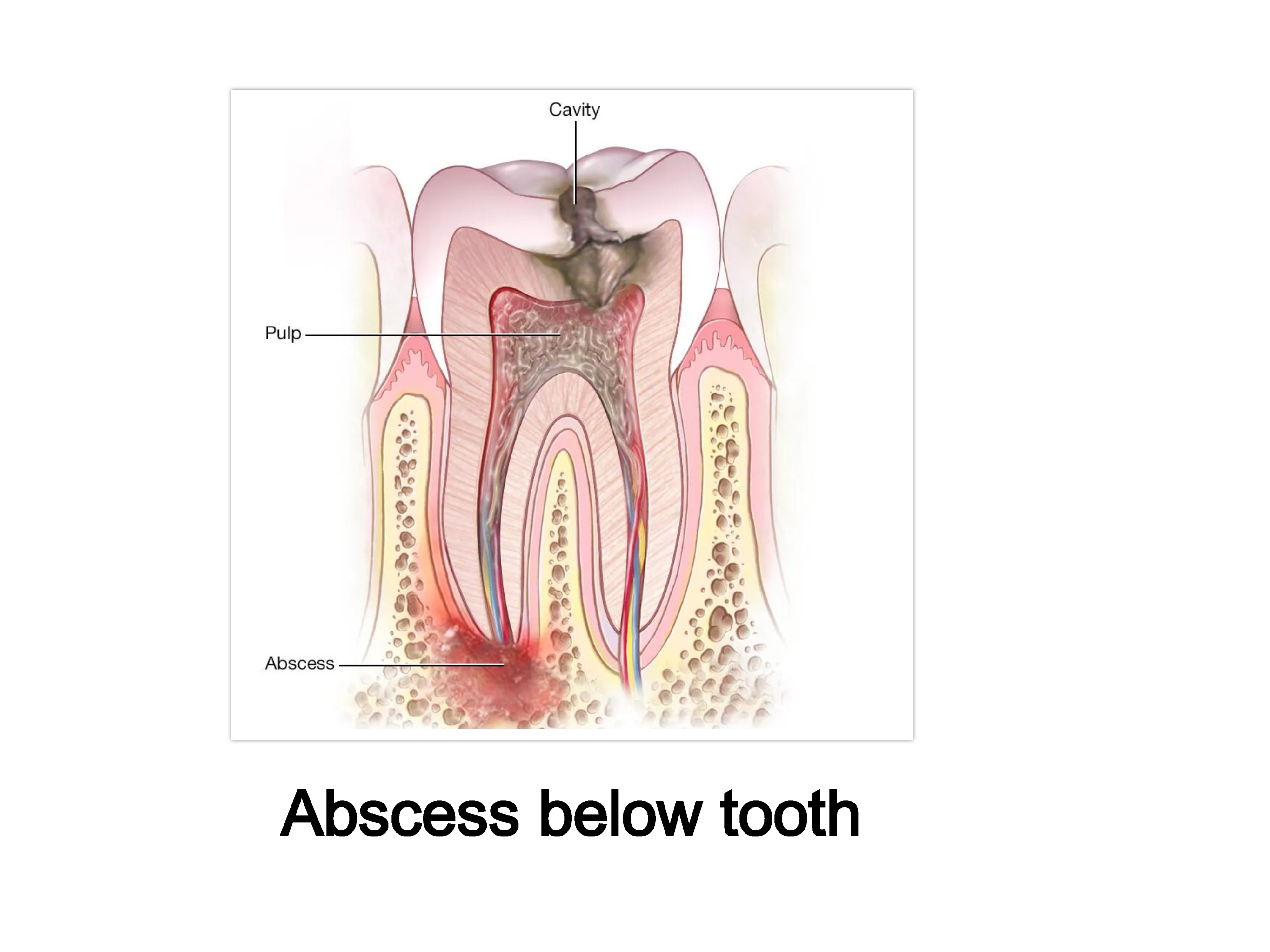
The dental pulp is the soft, living tissue located in the innermost part of the tooth. It is a highly vascular and innervated connective tissue that fills the pulp chamber (in the crown) and the root canals.
- Nerves: The pulp contains sensory nerves that transmit sensations of pain, temperature, and pressure to the brain.
- Blood Vessels: These provide the tooth with essential nutrients and oxygen and remove waste products, ensuring the tooth's vitality and health.
- Connective Tissue: This matrix supports the other components of the pulp.
- Odontoblasts: These specialized cells line the outer surface of the pulp and are responsible for forming dentin, the hard tissue that makes up the bulk of the tooth structure and surrounds the pulp.
- Defense Cells: The pulp also contains various immune cells that help protect the tooth from bacterial invasion and infection.
Pulp is a soft, living connective tissue containing nerves, blood vessels, and cells (like odontoblasts). It provides the tooth with sensation, nutrients, and the ability to form new dentin.
The dental pulp gets inflamed (a condition called pulpitis) primarily as a defense mechanism against irritants, most commonly a bacterial invasion resulting from untreated tooth decay. The pulp is encased in the rigid, unyielding walls of dentin and enamel, which means it has no room to expand when it swells, leading to increased pressure and pain.
- Tooth Decay (Cavities)
- Dental Trauma
- Repetitive Dental Procedures
- Worn Enamel
- Periodontitis
In essence, the pulp's inflammatory response is an attempt to protect the tooth's vitality. However, because the pulp is trapped within a confined space, the swelling and pressure often restrict its own blood supply, which can lead to irreversible damage and eventual pulp death (necrosis) if the source of irritation is not removed.
The severity of the inflammation determines if it is reversible (can heal with treatment) or irreversible (requires a root canal or extraction).
The dental pulp's "self-healing" capacity primarily refers to its ability to form a protective barrier of new dentin, a process called tertiary dentinogenesis (which includes both reactionary and reparative dentin formation). This healing process is a defense mechanism against external injuries like tooth decay, trauma, or wear, aiming to protect the vital inner pulp tissue from bacterial invasion and further damage.
- Stimulus: When decay or injury approaches the pulp, but before severe, irreversible inflammation sets in, the existing odontoblast cells are stimulated.
- Reactionary Dentin Formation: In cases of mild to moderate irritation where the original odontoblasts survive, they increase their metabolic activity and produce a localized, thin layer of new dentin called reactionary dentin along the existing pulp-dentin interface. This effectively thickens the dentin barrier.
- Reparative Dentin Formation: In more severe cases where the primary odontoblasts are destroyed or the pulp is exposed, a more complex process is triggered.
- Stem Cell Recruitment: Undifferentiated mesenchymal stem cells (also known as dental pulp stem cells, or DPSCs) residing deeper within the pulp tissue are activated.
- Differentiation: These stem cells migrate to the injury site, proliferate, and differentiate into new "odontoblast-like" cells.
- Dentin Bridge Formation: These new cells then begin to form a localized, often less organized, hard tissue matrix called reparative dentin, which forms a "dentin bridge" to seal the exposure site.
The term "self-healing" is conditional and has significant limitations:
- Requires Intervention: True self-healing (reparative) typically requires a dentist to remove the source of irritation (like the decay and bacteria) and place a protective material (like calcium hydroxide or mineral trioxide aggregate, MTA) over the exposed or near-exposed pulp to stimulate this process.
- Irreversible Damage: If the inflammation progresses to the "irreversible" stage, the pulp tissue's blood supply is often compromised, leading to pulp death (necrosis), and the tissue can no longer heal itself. In such cases, a root canal is necessary to save the tooth.
- Quality of Dentin: The newly formed reparative dentin may not be as perfectly organized or mechanically strong as the original primary dentin, sometimes containing "tunnel defects" that can potentially allow future bacterial penetration.
Both calcium hydroxide and Mineral Trioxide Aggregate (MTA) aid pulp healing by creating an environment that stimulates the pulp's inherent ability to form reparative dentin. Their mechanisms are similar, primarily driven by high alkalinity and the release of calcium ions, which signals the body's stem cells to differentiate into new dentin-forming cells.
Vital Pulp Therapies (VPT):
- Indirect Pulp Capping (IPC): Used when deep decay is very close to the pulp but hasn't exposed it. Most of the decay is removed, and a biocompatible material (like MTA or calcium hydroxide) is placed over a thin layer of remaining dentin to protect the pulp and encourage dentin repair.
- Direct Pulp Capping (DPC): This is done when the pulp is accidentally exposed (usually a tiny exposure less than 1mm) during cavity preparation or due to trauma in a tooth with minimal inflammation. A capping material is placed directly on the exposed pulp to promote healing and a protective dentin bridge formation.
- Pulpotomy: This procedure removes the inflamed or infected pulp tissue from the crown (the visible part) of the tooth, while leaving the healthy pulp within the roots intact and vital. It is very effective in children's primary teeth and is increasingly used in mature permanent teeth with certain types of inflammation.
Non-Vital Pulp Therapies:
These methods are for cases where the pulp inflammation is irreversible or the pulp has died (necrosis).
- Root Canal Treatment (RCT) / Pulpectomy: This is the most common treatment for irreversible pulpitis in permanent teeth. The entire pulp (from the crown down through all root canals) is removed. The inside of the tooth is thoroughly cleaned, disinfected, shaped, and then filled and sealed with a material called gutta-percha to prevent reinfection. The tooth usually requires a crown afterward for protection and strength.
- Tooth Extraction: If the tooth is too damaged to be saved by a root canal or the infection is too severe, the entire tooth must be removed. The patient can then explore replacement options such as a dental implant or bridge.