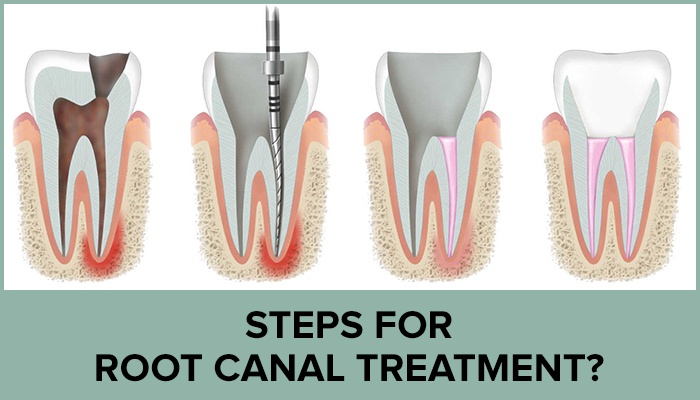
The dentist evaluates symptoms such as severe toothache, prolonged sensitivity to hot/cold, swelling, or the presence of an abscess. Dental X-rays are mandatory to view the shape of the root canals and determine if there are any signs of infection in the surrounding bone.
Local anesthesia is administered to completely numb the tooth, ensuring a painless and comfortable procedure. A rubber dental dam may be placed over the tooth to isolate it, keeping the area sterile and free of saliva during treatment.
If the tooth is heavily decayed or fractured, the dentist may use a drill to remove the compromised structure. This prevents the tooth from shattering under biting pressure during the procedure and prepares it for the eventual protective crown.
The dentist uses a small drill to create a precise access opening through the biting surface of the tooth (or the back of a front tooth). This provides a direct, straight-line path into the pulp chamber and the underlying root canals.
Using specialized, highly flexible endodontic files (often engine-driven rotary files), the dentist carefully removes the dead or infected pulp tissue, bacteria, and nerve fibers. The canals are widened and shaped to prepare them for the filling material.
Throughout the cleaning process, the root canal system is continually flushed and irrigated with powerful antimicrobial solutions (like Sodium Hypochlorite) to chemically dissolve debris and aggressively disinfect the microscopic tubules inside the roots.
Once thoroughly sterilized and dried, the empty canals are filled with a biocompatible rubber-like material called gutta-percha. This material, combined with an adhesive sealer cement, is packed tightly to hermetically seal the roots and prevent any future bacterial reinfection.
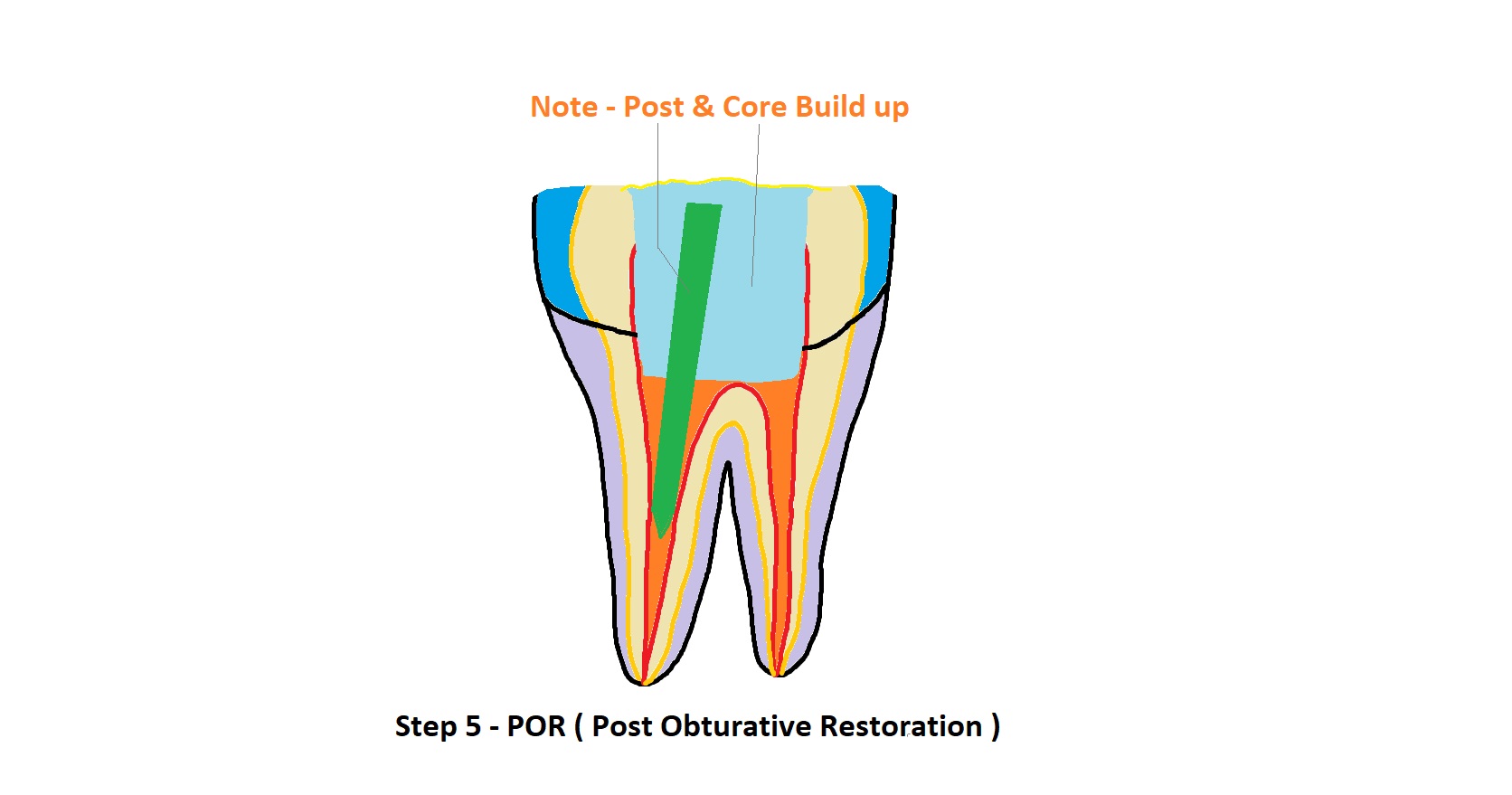
The access opening is closed using a strong composite resin. If the tooth has lost significant structure due to decay, a fiber or metal post may be inserted into the canal for added support, followed by a "core build-up" to replace the missing bulk of the tooth.
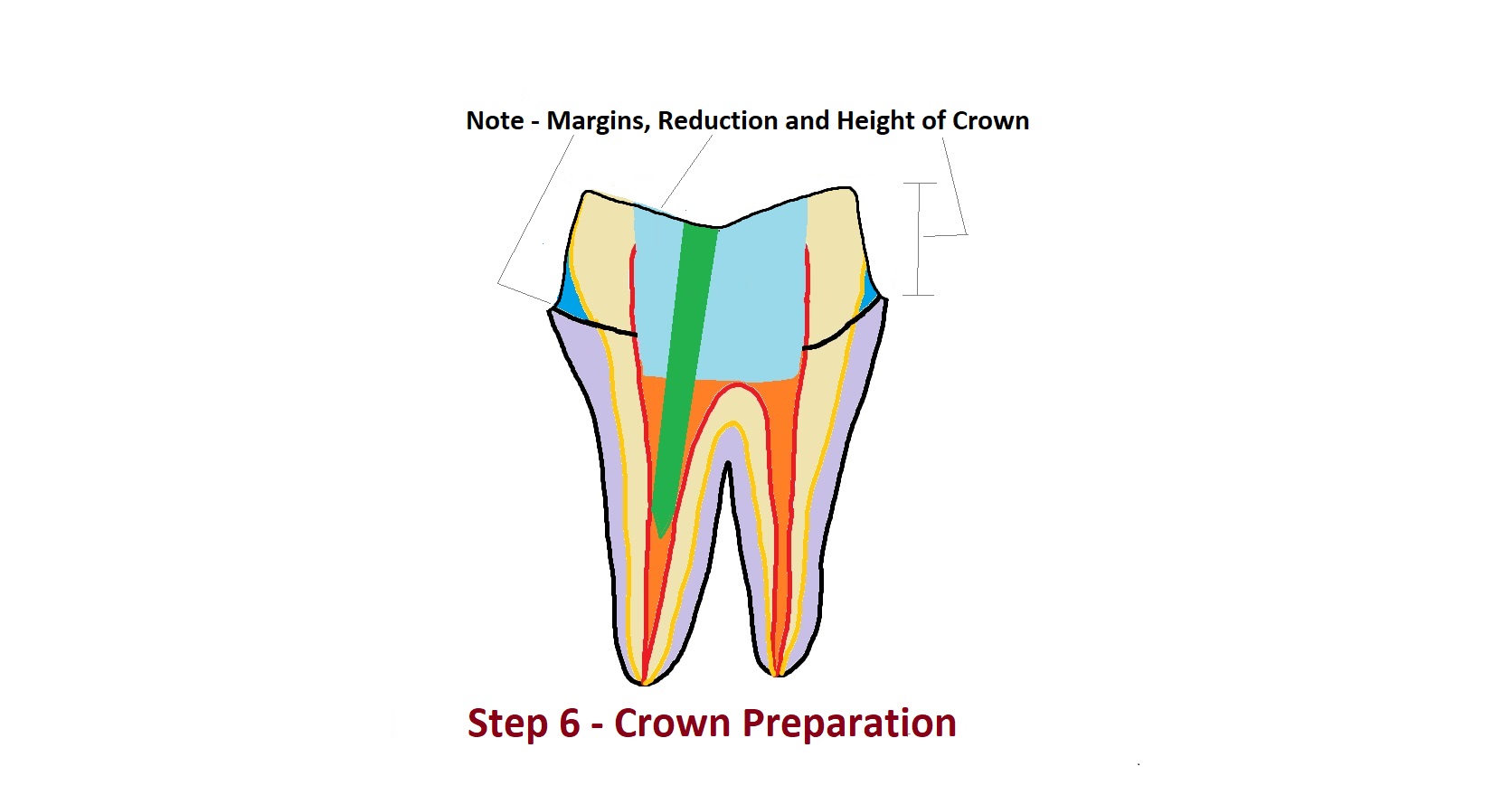
Yes. A tooth that has undergone a root canal becomes brittle over time because its blood supply is gone. A custom-fabricated dental crown is permanently cemented over the tooth to restore its strength, protect it from splitting, and return it to full chewing function.
Mild tenderness is normal for a few days as the bone heals, which can be managed with prescribed medications. Patients are advised to maintain excellent daily oral hygiene and return for 6-month check-ups to monitor the long-term success of the restored tooth.